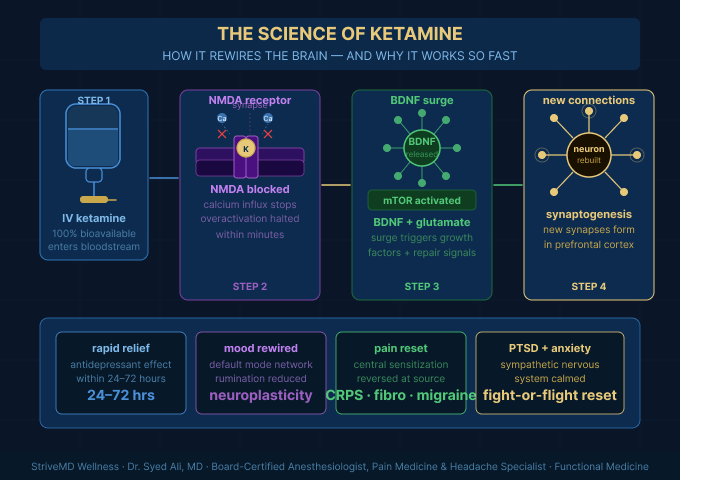
The Science Behind Ketamine — How It Rewires the Brain and Why It Works So Fast
By Dr. Syed Ali, MD — Board-Certified Anesthesiologist, Pain Medicine Physician, Headache Specialist, Functional Medicine Physician, and Oral Board Examiner for the American Board of Anesthesiology
If you have ever wondered why ketamine therapy is generating so much excitement in the medical community — and why patients who have struggled for ears with depression, PTSD, chronic pain, and anxiety are finally finding relief — the answer lies deep within the brain itself. As a board-certified anesthesiologist, pain medicine physician, headache specialist, and functional medicine physician, I have spent my career studying how medications interact with the nervous system at the most fundamental level. What ketamine does to the brain is nothing short of remarkable, and understanding the science behind it helps explain why it works faster, deeper, and more durably than anything we have had before.
The Problem With Conventional Antidepressants— Why They Take So Long
To appreciate what makes ketamine so different, it helps to first understand why traditional antidepressants fall short for so many patients.
Conventional antidepressants — SSRIs like sertraline and fluoxetine ,SNRIs like venlafaxine, and older tricyclic antidepressants — work primarily by increasing the availability of monoamine neurotransmitters like serotonin, dopamine, and norepinephrine in the synaptic cleft. The theory, known as the monoamine hypothesis of depression, has guided psychiatric treatment for over60 years.
The problem is that this approach is indirect, slow, and incomplete. These medications typically take four to six weeks to produce noticeable antidepressant effects — if they work at all. Research consistently shows that nearly two-thirds of patients with major depressive disorder do not achieve full remission with their first antidepressant, and a significant portion continue to struggle through multiple medication trials without adequate relief. For patients in the depths of a severe depressive episode, waiting weeks for a medication that may not even work is not just frustrating — it can be genuinely dangerous.
Ketamine works on an entirely different system, through an entirely different mechanism, and produces results on an entirely different timeline. Here is why.
The NMDA Receptor — Ketamine's Primary Target
Ketamine is primarily an antagonist of the NMDA receptor — the N-methyl-D-aspartate receptor — which is a type of glutamate receptor found throughout the brain and central nervous system. Glutamate is the brain's primary excitatory neurotransmitter, and NMDA receptors play a critical role in synaptic plasticity, learning, memory formation, and the regulation of mood.
In patients with treatment-resistant depression, PTSD, and chronic pain, NMDA receptors are believed to become overactivated in ways that contribute to the sustained negative neural patterns associated with these conditions. Excessive NMDA receptor activity drives a cycle of neurological dysfunction —disrupting synaptic connections, impairing the brain's ability to form new healthy pathways, and locking patients into rigid, painful patterns of thought, emotion, and pain perception.
When ketamine binds to and blocks NMDA receptors, it interrupts this cycle rapidly and powerfully. But the story does not stop there — and this is where ketamine's effects become truly extraordinary.
The AMPA Receptor and the Glutamate Surge
When ketamine blocks NMDA receptors, it triggers a compensatory surge of glutamate activity through a different pathway — specifically through AMPA receptors, another class of glutamate receptors. This glutamate surge activates a cascade of downstream molecular events that are now understood to be central to ketamine's antidepressant and neuroplastic effects.
The glutamate surge stimulates the release of BDNF — Brain-Derived Neurotrophic Factor — which is often described as fertilizer for the brain. BDNF is a protein that promotes the growth, survival, and differentiation of neurons. In patients with depression and PTSD, BDNF levels are typically significantly reduced, contributing to the neuronal atrophy and synaptic loss that characterizes these conditions. Stress, trauma, and chronic pain all suppress BDNF production — effectively starving the brain of the nourishment it needs to maintain healthy neural connections.
Ketamine reverses this process rapidly. The BDNF surge triggered by ketamine activates another critical pathway — the mTOR signaling cascade —which directly stimulates the synthesis of new synaptic proteins and the rapid formation of new synaptic connections in the prefrontal cortex, one of the brain regions most critically involved in mood regulation, emotional processing, and executive function.
Synaptogenesis — How Ketamine Physically Rebuilds the Brain
This is the mechanism that separates ketamine from every anti depressant tat came before it and explains why its effects can be felt within hours rather than weeks.
Within hours of a ketamine infusion, studies using advanced neuro imaging have demonstrated measurable increases in synaptic density in the prefrontal cortex. New dendritic spines — the tiny protrusions on neurons that form the physical substrate of synaptic connections — begin to grow. Neural circuits that had been functionally impaired by chronic stress, trauma, or depression begin to re-establish healthy connectivity.
This process is called synaptogenesis — the formation of new synaptic connections — and it is the neurobiological equivalent of rebuilding damaged infrastructure in the brain. Traditional antidepressants do not produce this kind of rapid structural change. Ketamine does, and it does so within a timeframe that is genuinely unprecedented in psychiatry.
As a functional medicine physician, I find this mechanism particularly compelling because it addresses the underlying neurobiological damage caused by chronic illness — not just the symptomatic surface of depression or anxiety. We are not simply adjusting neurotransmitter levels. We are facilitating the physical repair and regeneration of neural architecture.
The Default Mode Network and Ketamine's Effect on Rumination
One of the most fascinating aspects of ketamine's neurological effects involves what researchers call the Default Mode Network — a network of brain regions that is active when the mind is at rest, not focused on external tasks. In healthy individuals, the default mode network facilitates self-reflection, planning, and autobiographical memory. In patients with depression, PTSD, and anxiety disorders, the default mode network becomes hyperactive and dysregulated, driving the relentless negative rumination, intrusive memories, and self-critical thought patterns that define these conditions.
Ketamine has been shown to temporarily reduce the hyperactivity of the default mode network, creating what neuroscientists describe as a window of increased neuroplasticity — a period during which the brain is more receptive to forming new, healthier patterns of thought and emotional response. This is precisely why combining ketamine therapy with psychotherapy produces significantly better long-term outcomes than either treatment alone. The neuroplasticity window opened by ketamine creates an optimal opportunity for therapeutic work — allowing patients to process trauma, challenge negative beliefs, and establish new cognitive patterns in a way that the brain can more readily absorb and sustain.
Why Ketamine Works So Fast — The Timeline Explained
The speed of ketamine's antidepressant effect is perhaps its most clinically significant feature, and it is directly attributable to the mechanisms described above.
Traditional antidepressants require weeks because their effects depend on gradual downstream changes in gene expression and receptor sensitivity — slow, indirect processes that unfold over time. Ketamine bypasses all of that. By directly blocking NMDA receptors, triggering the glutamate surge, releasing BDNF, activating
To learn whether IV ketamine therapy is right for you, contact StriveMD Wellness to schedule a personal consultation with Dr. Syed Ali.

